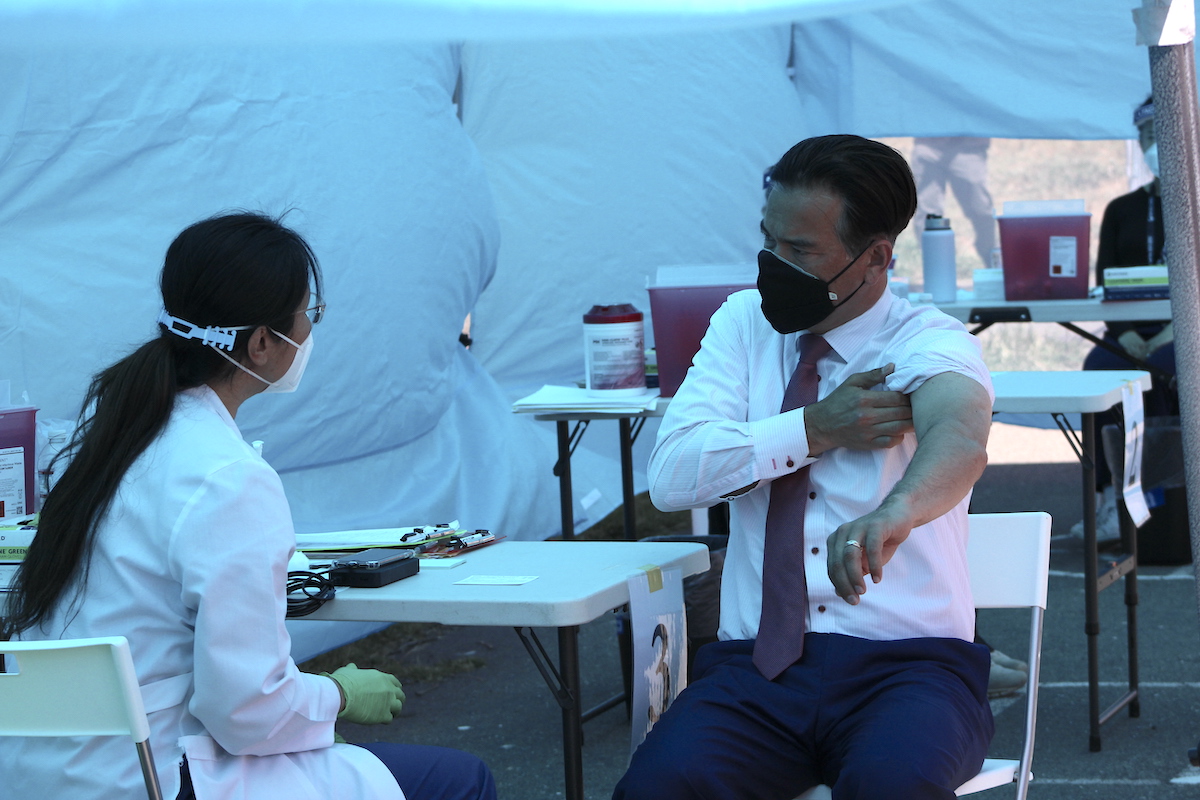
Under a blue tent at Madison Park in Oakland on Thursday, California Assemblymember Rob Bonta rolled up the left sleeve of his white dress shirt and looked away as Dr. Kimberly Chang, a physician with Asian Health Services, poked him with his first shot of the Moderna vaccine.
“I tried not to look at the needle. It’s not because I’m afraid of needles, I just don’t like to look at the needle,” Bonta—who represents Oakland, Alameda, and San Leandro—said afterward. “It was easy. It was painless. It was quick.”
On April 15, Bonta and millions of other Californians over the age of 16 became eligible for a vaccine, regardless of profession, location, or health status. The expansion of vaccine eligibility to all adults comes as nearly half of California’s residents 16 and older have already received at least one dose of a COVID-19 vaccine, according to Governor Gavin Newsom.
“It’s safe. It’ll protect you. It’ll protect your family. It’ll protect your community. It’ll protect those you love,” Bonta, who was served by Asian Health Services as a child and is also nominated to be the next California attorney general, said of the vaccine.
In Alameda County, more than 1.1 million vaccine doses have been administered and nearly 56% of the county’s residents over the age of 16 have received at least one dose. About 35% of county residents are fully vaccinated, according to the latest numbers posted on the county’s public health department dashboard. Oakland’s numbers are nearly similar to the county overall.
The vaccination sites hosted by community groups like Asian Health Services, Native American Health, and La Clinica, just to name a few, have been providing targeted local pop-up clinics to ensure that the vaccine is equitably distributed to low-income and communities of color.
Community clinics and trusted messengers have been key to equitable vaccine distribution
Inequities in vaccine distribution are evident at mass vaccination sites, including the Oakland Coliseum, according to the latest numbers released from California’s Office of Emergency Services. In the walk-up and drive-thru lines, nearly 41% of the shots have been administered to white people and more than 28% to Asian Americans. Less than 18% were given to Latinos and less than 4% were given to Black people, even though Latinos and Black people make up 22% and 10% of Alameda County’s population, respectively, and a much higher proportion of East Oakland.
At mobile clinics where vaccine allotments from the Federal Emergency Management Agency were used to target those more at risk from COVID-19, numbers better reflected Oakland’s diversity: nearly 26% were Latino, more than 20% Black, more than 23% Asian, and just over 23% white.
Greg Garrett, chief operating officer at Native American Health, said it takes different strategies to reach people in the “cracks and crevices” of the community, including those with language barriers, little to no access to the technology needed to make a vaccine appointment, and hesitancy towards the vaccine. That’s where “warm handoffs” from those with connections in specific communities can help others get their shots.
“In reality, those people wouldn’t be vaccinated otherwise,” Garrett told The Oaklandside.
Observations from San Francisco health officials published in a recent issue of the New England Journal of Medicine’s Catalyst highlights a “cautionary tale,” where healthcare workers found online scheduling—like the state’s MyTurn site—attracted more affluent people rather than older patients at greater risk of complications from COVID-19.
“Successful interventions to vaccinate diverse people have included communication through text, telephone, and mass media, and the establishment of drop-in vaccine sites,” the San Francisco physicians and nurses concluded.
In Oakland, workers at the Center for Empowering Immigrants and Refugees helped vaccinate 60 of their clients and as word spread about this assistance, the need for more clinics arose, Garrett said.
Homies Empowerment—which serves the recently incarcerated, immigrants and others—combined their vaccination efforts to their food drive, allowing them to give out 150 doses in four hours along with bags of groceries.
“It’s all about building trust,” Garrett said.
Supply problems could reemerge because of Johnson & Johnson’s vaccine pause
One setback to vaccine trust came Tuesday, when the U.S. Centers for Disease Control and Prevention and the Food and Drug Administration published a joint statement recommending that the use of the one-shot Johnson & Johnson vaccine be paused. That was due to an “extremely rare” and severe type of blood clot that occurred in six American women after 6.8 million doses had been administered in the United States.
Besides only requiring one dose, the Johnson & Johnson vaccine didn’t need to be kept as cold as the Pfizer and Moderna vaccines, making it easier to transport and less likely to be wasted if doses were thawed and not immediately used.
Brian Ferguson with Cal OES said they didn’t anticipate the pausing of the one-shot vaccine to affect operations at the Oakland Coliseum because they shifted back to using Pfizer as of Sunday, April 11, when FEMA’s role there ended and Alameda and Contra Costa counties took over.
As of April 12, Alameda County had received 41,100 doses of the Johnson & Johnson shot, compared to about 284,000 and 239,000 doses of the Pfizer and Moderna vaccines, respectively, according to the Alameda County’s vaccine dashboard.
But Garrett says not having the option of the Johnson & Johnson shots means people now have to return for a second dose, which is primarily of Moderna. Native American Health also had to cancel two mobile clinics until more supplies can be delivered.
“It’ll cut our vaccine efficiency in half,” he said.
Now that the eligibility floodgates have opened, vaccine availability has become the major challenge to reaching herd immunity.
A report published this week by the U.S. Government Accountability Office found that because projecting future availability of vaccine doses can be difficult, “managing public expectations is critical” and should be done so through “timely, clear, and consistent communication about vaccine availability” “to ensure public confidence and trust.”
Dr. Rita Ng, head physician at Kaiser Permanente Oakland, said during a Facebook live event with The Oaklandside this week that all three vaccines have been in short supply, and every country, state, and county are vying for more doses.
“The vaccine supply is our greatest limiting factor at this point,” Ng said.
At a press conference in Union City on Thursday, Gov. Newsom proudly stated that more than 24 million doses of a vaccine would have been given to Californians by the end of the day.
Of those doses, 4.9 million were administered in the hardest hit communities in the state, including several zip codes in Oakland and Alameda County. Newsom reiterated the state’s pledge that 40% of vaccine doses coming into California would continue to go to people in communities that unfairly have borne the brunt of the pandemic.
With the state partnering with 337 community organizations and “trusted messengers,” Newsom said equity would remain at the center of the state’s vaccine plan.
“It’s been stubborn, it’s been hard, but it’s been foundational,” said Newsom.